Surgery for Liver Mets
 Liver metastases occurs when tumors spread to the liver from other areas of the body. The liver provides a fertile soil for metastatic spread because of its rich blood supply that promotes cell growth. A multidisciplinary treatment team is essential for treating liver tumors. A surgeon is a critical part of that team, and even if surgery isn’t an option initially, will monitor your progress and assess if there is an optimal time for surgical intervention. Numerous surgical techniques play an integral role in treating liver metastases.
Liver metastases occurs when tumors spread to the liver from other areas of the body. The liver provides a fertile soil for metastatic spread because of its rich blood supply that promotes cell growth. A multidisciplinary treatment team is essential for treating liver tumors. A surgeon is a critical part of that team, and even if surgery isn’t an option initially, will monitor your progress and assess if there is an optimal time for surgical intervention. Numerous surgical techniques play an integral role in treating liver metastases.
Minimally Invasive Liver Surgery
MILS has become the standard in the field of liver surgery in many centers. Conventional open liver surgery has not been replaced completely, as it is currently still used in cases of large tumors and complex vascular and biliary reconstructions. However, vast experience has been gained in MILS, and continue to extend boundaries and indications, along with the constant development of further technical advances, such as robotic surgery.
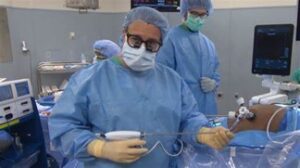
daVinci Robot Surgical System
One of the latest, most technologically advanced surgical tools available today is the daVinci Robot Surgical System. The daVinci Robot allows surgeons to provide minimally invasive procedures by displaying an enlarged, 3D and HD image of the surgical site and utilizing miniaturized tools inserted through a small incision to perform the surgery. Benefits to the daVinci system include minimal pain, an almost scarless surgery, low blood loss, a fast recovery and more.
Liver Resection
The tried and true way to deal with liver mets is by surgical resection. The hope is to remove the tumors and leave no microscopic cancer cells behind. A margin of normal tissue is included in the resected specimen. Unfortunately, surgery is only possible in a small percentage of patients who have liver tumors. Still, surgery is “gold standard” today against which other treatment plans are measured. This is an important part of the treatment plan of the patient who is a candidate. Both for hepatocellular carcinomas and for some cancers metastatic to the liver, surgical resection is a mainstay.
- What is a liver resection?
- A liver resection is when a section of the liver is removed by surgery. This surgery is performed as a treatment option for some cancers of the liver. It may also be performed on those willing to donate part of their liver to a loved one for organ donation. The liver is a vital organ and the onlly one that has the ability to regenerate itself. Up to 75% of the liver can be removed as long as the remaining liver tissue is healthy.
- What do I need to do before surgery?
- You will need to contact your insurance company to ensure that coverage and determine if a referral is required. A nurse will review your chart and confirm that all paperwork is in order. You will be taken to a pre-operative room, and an anesthesiologist will start an IV. Before any medications are administered, your surgeon will verify your name and the type of procedure you are having. You will then be taken to the operating room. After the appropriate form of anesthesia is administered, the surgery will be performed.
- What type of anesthesia will be used?
- You will have a pre-op interview with an anesthesiologist who will ask you questions regarding your medical history. A liver resection is usually performed under general anesthesia, which will keep you asleep during surgery.
- What happens during surgery, and how is it performed?
- An incision is made in the abdomen just below the rib cage. Your surgeon will carefully dissect the section of liver that is to be removed from the many veins, arteries, and bile ducts that support it. Once complete, the incision is closed with staples.
- What happens after surgery?
- Once the surgery is completed, you will be taken to a post-op or recovery room where a nurse will monitor your progress. It is important that your bandages be kept clean and dry. You may experience mild discomfort at the incision site, so your physician may prescribe pain medication.
- How long will I be in the hospital?
- Most patients will remain in the hospital for a week following a liver resection.
- What are the risks associated with a liver resection?
- As with any surgery, there are risks such as infection, or an adverse reaction to anesthesia. Your surgeon will inform you of the risks prior to surgery.
- What should I watch out for?
- Be sure to call your doctor if any of the following symptoms appear:
- Abdominal Pain
- Fever
- Nausea or vomiting
- Redness or swelling around the incision
- Upper back pain on the right side
- Warmth around the incision
- Will there be scar(s)?
- A scar will remain where the incision was made. It should fade and be less visible over time.
- When can I return to work and/or resume normal activities?
- Light activity at home is encouraged after surgery. You can expect to return to normal activities such as showering, driving, walking up stairs, light lifting, and work as soon as you feel comfortable. If you are taking narcotic medications for pain, you should not drive.
Liver Transplant
What is a liver transplantA liver transplant is the replacement of a sick liver with a donated, healthy liver. Liver transplants require that the blood type and body size of the donor match the person receiving the transplant.
Why do I need a liver transplant?
A liver transplant is necessary when your liver fails and a doctor recommends you be evaluated for a transplant. Transplants are available for some candidates who have primary liver cancer, metastatic colorectal cancer, and metastatic neuroendocrine cancer.
If primary liver cancer is involved and you are a candidate or if you have liver damage that is severe enough from liver disease, transplantation may be necessary. A transplant provides you with a liver that can keep up with the demands of a full, active life.
Am I eligible for a transplant?
After being referred by a doctor to a transplant center, the transplant team evaluates your overall physical and mental health, plan to pay for transplant related medical expenses, and emotional support family and friends will provide. Based on the findings, the team decides if you are eligible for a liver transplant.
The following procedures help in evaluating your health status:
- Blood tests – The patient’s blood count, blood and tissue type, blood chemistries, and immune system function will all be checked. In addition, blood tests for certain infectious diseases will be performed.
- Chest x-ray – Determines the health of your lungs and lower respiratory tract.
- Cholangiogram – Reveals any obstructions or growths in your bile ducts.
- CT (CAT) scan – This computerized image will show the size and shape of the patient’s liver and major blood vessels.
- Electrocardiogram (EKG or ECG) – Determines how well your heart is working and may reveal heart damage that was previously unsuspected.
- Gallium, colloidal gold, or technetium scan – Gives the transplant physician a view of your liver, gallbladder, and pancreas.
- Hepatic angiograph – Dye injected into your arteries will enable the transplant physician to see if there are any abnormalities or blockages in your blood vessels.
- Lower GI series – Ensures that you are free of intestinal abnormalities.
- MRI (magnetic resonance imaging) – May be used in place of CT scan or ultrasound to see inside the patient’s body.
- Peritoneoscopy – By inserting a flexible tube through a tiny incision in your abdomen, the transplant physician will be able to see any structural changes in the liver.
- Pulmonary function test – You will be asked to breathe into a tube attached to a measuring device, which will reveal how well your lungs are working and determine his blood’s capacity to carry oxygen.
- Renal function studies – Urine may be collected from you for 24 hours in order to determine if the kidneys are working correctly. Blood tests such as serum creatinine are also performed to measure kidney function.
- Total-body bone scan – If the patient has a liver tumor, ensures that it has not spread to any other part of the body.
- Ultrasound with Doppler examination – Determines the openness of the bile ducts and major vessels. It is commonly done in all liver transplant recipients before and after transplantation.
- Upper gastrointestinal (GI) series – This will show whether your esophagus and stomach are disease free.
If you are eligible, the center will add you to the national transplant waiting list. The waiting list is prioritized so the sickest people are at the top of the list.
Who is on the transplant team?
- YOU
- Dietician
- Floor or Staff Nurse
- Nurse Practitioner
- Pharmacist
- Physical Therapist
- Psychologist / Psychiatrist
- Social Worker
- Transplant Coordinator
- Transplant Physician (Hepatologist)
- Transplant Surgeon
- Your support team
How long will I have to wait for a liver transplant?
The waiting time for a liver transplant varies from person to person. The time you have to spend on the waiting list depends on your blood type, body size, stage of liver disease, overall health, and the availability of a matching liver. Days and weeks may pass while the transplant team waits for UNOS to locate the right liver for you. The anxiety and hope for the telephone to ring often becomes intense; the telephone a life preserver always at hand. Use this time to prepare for the hospital stay, get your support team organized, and arrange for help after surgery.
When the important call comes
- When the life-changing call comes, you should bring the following to the hospital:
- A list of your drug allergies
- Your health insurance information
- Your medications
IMPORTANT: As soon as a liver is available, you should stop all eating and drinking immediately. Your stomach must be empty when you are taken into the operating room.
What should I expect when I arrive for my new liver?
After admission, you will undergo a thorough physical examination, including more blood work, a chest x-ray, and EKG, and, possibly, other tests. Unfortunately, surgery may be postponed in some cases. You will be sent home if:
- The donor liver shows signs of deterioration or poor function
- You have an infection
- You have any other medical problem that would interfere with surgery or recovery
If surgery is postponed, the transplant team can help you through the disappointment. This is only a temporary setback, and the search for a new liver will go on.
What happens before my transplant?
You may receive an enema to clean out your intestines and prevent constipation after surgery. Your chest and abdomen will be shaved clean to prevent infection, and an intravenous (IV) line will be inserted in your arm or just under your collarbone to give medication and keep you from getting dehydrated. You will also be given a sedative to help you relax and feel sleepy before going to the operating room.
What happens during the transplant?
You will be under general anesthesia throughout the surgery. Once asleep, the transplant surgeon will make an incision shaped like a boomerang on the upper part of the abdomen. The surgical team will then remove your old liver, leaving portions of your major blood vessels in place. The new liver will then be inserted and attached to these blood vessels and to your bile ducts. To help with bile drainage, a tube will also be inserted in the bile duct during surgery. Your transplant will take between four and twelve hours.
Will I have to have drains and tubes?
During liver-transplant surgery, the surgeon may find it necessary to place a small tube, called a T-tube, into your bile duct. The T-tube allows bile to drain out of your body into a small pouch, known as a bile bag. The amount of bile, which varies in color from deep gold to dark green, can then be measured. If a T-tube is put in place, it may remain attached to a bile bag for a week or possibly longer. When the bile bag is removed the T-tube will be tied or capped. It will remain in place for several months so that it can be used for special testing.
The T-tube is attached to the skin with a stitch. The dressing around the tube should be changed at least once daily, and more often if it becomes moist. The transplant nurse will show you how to change the dressing without pulling out the T-tube.
Other drains may be placed in your abdomen during the postoperative period. A common name for these drains is Jackson-Pratt (JP). They are used to drain fluid from around the liver. Generally, these drains are removed before you go home.
How will I feel after surgery?
You will wake up in the intensive care unit after the anesthesia wears off. You will have some pain and/or discomfort but will be given medication to help give you relief. You will have a tube inserted through your nose which runs down your throat and into your stomach. This will keep your stomach empty and help to prevent nausea and vomiting. You may also have a tube inserted in your throat to help you get enough oxygen. It will be connected to a breathing machine called a ventilator. You should try to relax and let the machine breathe for you. You will not be able to talk with this tube in place, but will only need it for a few days. Nurses will do everything they can to help you patient communicate. Afterwards, your throat may feel sore or scratchy for a few days.
You will be asked to cough periodically to keep your lungs clear. If it hurts to cough, you should ask for someone to support your abdomen or hold a small pillow close. You will have an IV line in your arm or neck under the collarbone, which will be used to give fluids and medication for the first few days after surgery.
For several days after surgery, you will have a catheter in your bladder to drain urine. You may feel uncomfortable, and may feel that you have to urinate constantly, but it is only temporary. During surgery, several drains will be placed in or near the incision. These drains will be removed 5 to 10 days after surgery.
The length of a hospital stay will depend on your progress. You will be encouraged to talk to someone on your transplant team if you are uneasy or apprehensive about going home.
When will I follow up?
After leaving the hospital, you will receive a schedule of follow-up clinic visits for lab tests and checkups. The purpose is to track your progress and detect potential complications as early as possible. On days when you are scheduled for follow-up visits, you should bring your medication list and your surgery handbook. You will be given specific instructions for routine lab work or special tests.
Do I need to watch for anything?
While primary concerns involve infection and rejection, many other problems, such as colds or flu, adjustment of other medications, and minor infections can be handled by a local physician. You need to take precautions and learn to watch for signs of infection and rejection that necessitate notifying a local physician or transplant team immediately. These include:
- a cough that produces a yellowish or greenish substance
- a dry cough that continues for more than 1 week
- a fever that continues for more than 2 days
- a rash or other skin changes
- an inability to take prescribed medication
- bleeding, bruising, black stools, red or rusty-brown urine
- burning discomfort with urination
- emergency-room treatment or hospitalization
- exposure to mumps, measles, chicken pox, or shingles
- pain, discharge, or swelling at the T-tube site
- prolonged nausea, vomiting, or diarrhea
- shortness of breath
- unusual weakness or light-headedness
- vaginal discharge or itching
United Network of Organ Sharing (UNOS)
Every patient waiting for an organ transplant in the United States is registered in the UNOS computerized data network. All have equal access to donated organs. The 68 organ recovery organizations across the country are members of UNOS.
When an organ procurement organization coordinator contacts UNOS, the UNOS technician inputs the organ donor’s medical history, physical measurements, and blood type, and prints a computerized list of likely transplant recipients. The list is printed in order of matching priority, which includes medical criteria, length of time waiting, blood type, body weight, size of recipient diseased organ, and severity of illness. Kidney and pancreas recipients are also matched by tissue (genetic) typing.
If the first potential recipient does not match medically with the available organ, the OPO coordinator maintains the computer search in an assigned region or elsewhere in the nation for a potential recipient who most nearly matches the donor. Likewise, organ recovery organizations throughout the United States will notify each other when an organ becomes available for waiting recipients in their respective areas.
Matching donor organs with recipients is critical. Transplant waiting times may vary from a few months to several years because of matching difficulties.
What are the risks of a liver transplant?
The most common risks associated with liver transplants are rejection. Rejection occurs when your body’s immune system attacks an object it does not recognize. To prevent rejection, you will be given medicines to weaken the immune system. Modern medications have made rejection less of a concern in liver transplant patients.
Rejection medications may have side effects of increased blood pressure, headaches, diarrhea, and nausea. Also, because rejection medications weaken the immune system, it can be hard for you to fight infections. However, most infections can be treated with medications.
Helpful Resources
Liver Transplant Sources
American Liver Foundation
1425 Pompton Avenue
Cedar Grove, NJ 07009
(201) 256-2550
(800) 223-0179
International Transplant Nurses Society
Foster Plaza 5, Suite 300
651 Holiday Drive
Pittsburgh, PA 15220
(412) 928-3667
Transplant Recipients International Organ (TRIO)
1735 I Street NW, Suite 917
Washington, DC 20006
(202) 293-0980
(800) 874-6386
United Network for Organ Sharing (UNOS)
The National Organ Procurement and Transplantation Network
1100 Boulders Parkway, Suite 500
P.O. Box 13770
Richmond, VA 23225-8770
(804) 330-8500
What can people do to help those who need a liver transplant?
People can help by registering to be an organ donor. To obtain an organ donor card, please visit: www.organdonor.gov.




